The idea of being able to control devices using only the power of our minds has long captured the imagination, but with research underway at a British university, ‘telekinesis’ might soon rise from the pages of fiction.
The Next Generation Neural Interfaces (NGNI) Group at Imperial College London’s Centre for Bio-Inspired Technology has a specific focus on the design and development of mechanical architectures and insertion methods for millimetre-scale wireless neural probes.
It’s estimated that if we were able to record electrical activity simultaneously from between 1,000 and 10,000 neurons, with the signals deciphered using machine learning AI, that this would enable useful prosthetic control.
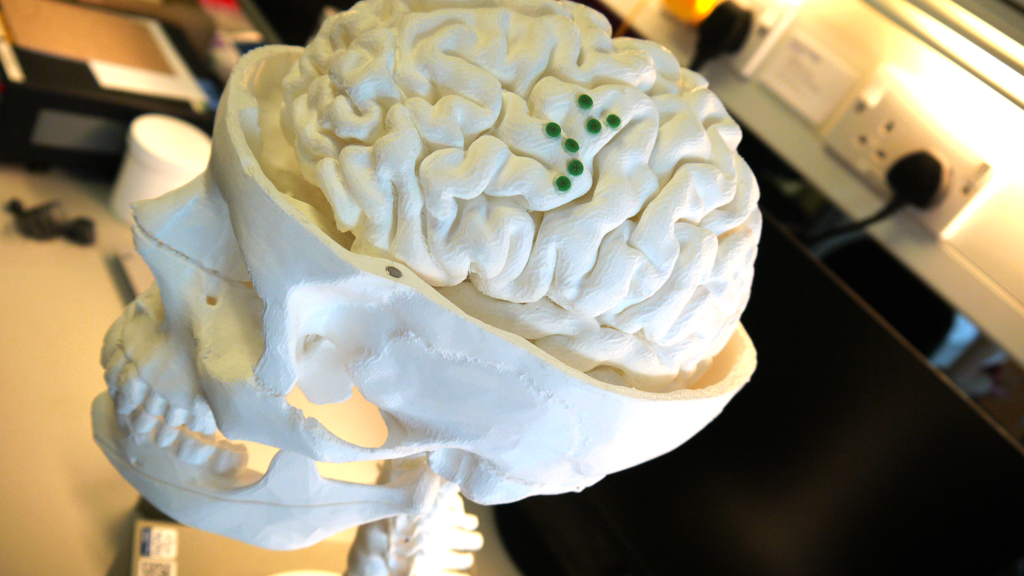
The current research project is presented to us on a model human skull by Matthew Cavuto, NGNI team member and ‘lab mechanical engineer’, as he modestly puts it.
Taking sections of skull bone away, he shows us NGNI’s prototype neural probe concept, each tiny disk sat independently on top of the exposed brain matter.
Present-day neuro interface devices – like the Utah Array or the Michigan Probe – are formed of 64 spikes in a rigid grid formation, with a big wire bundle running off it, and bring a wide range of problems.
The physical tether means there’s an instant root for infection, and because the probes are rigid, there’s a high rejection rate due to the trauma they cause when in situ.
“The biggest issue today with neural interfaces is the rejection and loss of long-term fidelity recording,” explains Cavuto. “What our group is doing is designing a wireless neural interface, where the probes themselves communicate through the skull to a receiver that’s on the outside.”
The probes are placed across the brain individually and left free to move with it, and have no onboard electronics, only 8 microwires, each 20 microns in diameter, thinner than a human hair.
“They’re quite flexible, so they cause minimal trauma. Once you get below 25 microns, you’re no longer able to puncture the microvasculature of the brain, and the key to avoiding rejection is to avoid any bleeding,” Cavuto explains.
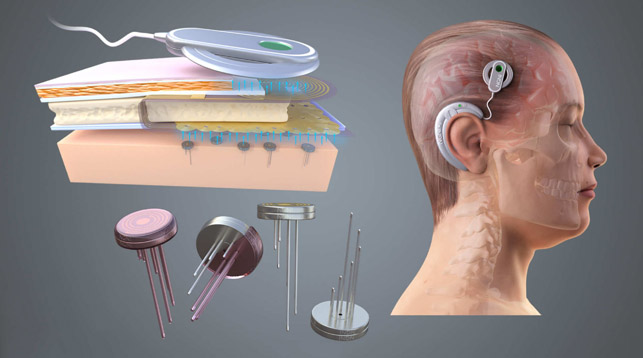
The skull is then resealed with a piece of artificial bone, and a device attached to the outside of the skull, similar in appearance to a cochlear implant, can send and receive the signals from the probes.
The go-to guy for researchers
Cavuto is the go-to for researchers in the NGNI group and their neighbouring Lab On A Chip counterparts who need concept ideas designed and made physical.
With an undergraduate degree from the Massachusetts Institute of Technology, majoring in mechanical engineering concentrating in Biomechanics and Biomedical Devices, and an MSc in Biomedical Engineering at Imperial College, Cavuto is now undertaking an MPhil in Electrical and Electronic Engineering and continuing his research on the NGNI team.
“Everything here is custom made components,” he explains, walking us around the lab. The space is filled with projects he’s worked on, but many of which are too secretive to be talked about in public. They vary from rugged casings for electronic devices, handheld medical tools, down to the delicate 4mm probe mock-ups.
“Prototyping is really difficult with this scale,” says Cavuto, holding one of the prototypes under a microscope to show us tracks in a part that then channel into 100-micron holes.
These parts, like nearly all the parts on show in the lab, are 3D printed on the lab’s 3D Systems Figure4.
Having initially looked at 3D Systems’ large ProJet 7000 SLA machines, Cavuto and the team were surprised by the part quality and speed of the smaller Figure4, which uses non-contact membrane digital light printing (DLP).
The technology allows for very fast print output, while still maintaining the high detail of the SLA process, with a range of resins offering varying mechanical properties.
It’s clear that the rapid nature of developing ideas into a physical form plays a big part in developing the lab’s latest ideas. Concepts are typically given to Cavuto as basic sketches or a series of measurements, before he designs an initial 3D CAD model in Solidworks.
Once that’s checked over, it moves into 3D Systems’ 3D Sprint build software and onto the printer.
“If I’m checking what the ergonomics feel like I’m not going to know from the CAD immediately if this is the right shape,” he says. “So, I print it in an hour, cure it for an hour, I can feel it, go change it in CAD and print it again. And I can do that three times in a day, and have something the way that I want it.”

Neural interface – ten minutes to print
For the implant nodes, it takes just 10 minutes to print 64 of them on the Figure4, at a 10-micron resolution. At the other end of the scale is the 15:1 scale model of a probe.
Used when presenting the NGNI’s work at conferences, it helps explain to people how the system will work on a scale that’s more manageable.
3D-printed in Cavuto’s favourite Tough GRY-15 material, in addition to the speed and detail of the print, its designer also loves the surface finish that requires very minimal post processing. As he puts it, laughing: “I’m doing so many different projects for so many different people that I don’t really have time!”
Cavuto is full of insights into the 3D printer’s abilities – having worked previously with a wide variety of additive and traditional manufacturing technologies.
For example, the Figure4 has a relatively small build volume (124.8 x 70.2 x 196 mm), yet because of the nature of the DLP printer, he has found the orientation of the part is not as important for finish quality, giving the user more freedom when arranging the build area layout.
A feature in the printer’s accompanying 3D Sprint software will automatically split up any parts too big for the build area, adding pin and hole joins.
“The supports on this printer can be ridiculously tiny,” says Cavuto. “You can print down to 10 microns layer height, and the supports can be extremely minimal, which has been useful to us when making these small parts.”
The next stage is testing 3D Systems’ latest biocompatible materials, which should help speed up elements like certification, and aid other developments the lab is working on, such as advancements in microfluidics – described as shrinking a whole lab down into a small package for testing things like blood samples.